Florida, often celebrated as the Sunshine State, is a magnet for travelers, retirees, and families seeking new beginnings or extended stays. From the vibrant nightlife of Miami to the magical theme parks of Orlando and the serene beaches of Key West, its diverse landscapes and rich culture offer an unparalleled lifestyle. Many who visit find themselves captivated, considering a permanent relocation or a longer-term residence. Whether you’re planning a move, an extended family trip, or looking for a comprehensive guide to local amenities and lifestyle shifts, understanding essential services like healthcare is paramount. For individuals and families with limited income, navigating the healthcare landscape can seem daunting, but thankfully, programs like Medicaid are designed to provide crucial support.
Medicaid in Florida offers a lifeline, ensuring access to vital medical care for eligible low-income residents. While often perceived as a complex system, understanding its framework and application process is a crucial step towards securing your well-being in this beautiful state. For those exploring long-term accommodation options, perhaps considering an apartment in Tampa or a villa near Jacksonville, integrating into the local community involves more than just finding the perfect spot; it means ensuring peace of mind for your health needs. This guide aims to demystify the process of signing up for Medicaid in Florida, offering clarity and practical steps to help you or your loved ones access necessary medical coverage as you embrace the Florida lifestyle.

Understanding Medicaid in the Sunshine State
Medicaid is a joint federal and state program that provides health coverage to millions of Americans, including children, pregnant women, parents, seniors, and individuals with disabilities. In Florida, the program is administered by the Agency for Health Care Administration (AHCA) and plays a pivotal role in ensuring that low-income residents have access to comprehensive medical care. Unlike some other states, Florida has not expanded its Medicaid program under the Affordable Care Act (ACA), meaning eligibility is primarily tied to specific categories of need beyond just income. This distinction is vital for anyone considering moving to or living long-term in the state.
For many, the idea of settling into a new destination like Florida conjures images of pristine beaches, vibrant cities, and world-class attractions such as Walt Disney World Resort or the historic streets of St. Augustine. However, the practicalities of daily life, especially healthcare, are an equally important consideration for a seamless transition. For families embarking on extended stays or individuals planning to make Florida their permanent home, understanding the safety net that Medicaid provides can alleviate significant financial burdens related to medical emergencies, routine check-ups, and ongoing treatments. It’s an essential component of responsible planning, much like researching the best resorts for a family trip or the most suitable long-term accommodation options. Knowing that essential health services are accessible offers a sense of security, allowing residents to fully immerse themselves in the enriching experiences Florida has to offer, from exploring Everglades National Park to enjoying the cultural vibrancy of South Beach.
Who Qualifies? Eligibility Criteria for Florida Medicaid
Eligibility for Medicaid in Florida is determined by a combination of factors, including income, household size, and specific circumstances or categories. Since Florida has not expanded its Medicaid program, qualifying typically requires fitting into one of several defined groups beyond simply having a low income. This makes understanding the specific criteria crucial for prospective applicants. The process is designed to support the state’s most vulnerable populations, offering a vital safety net for their health needs.
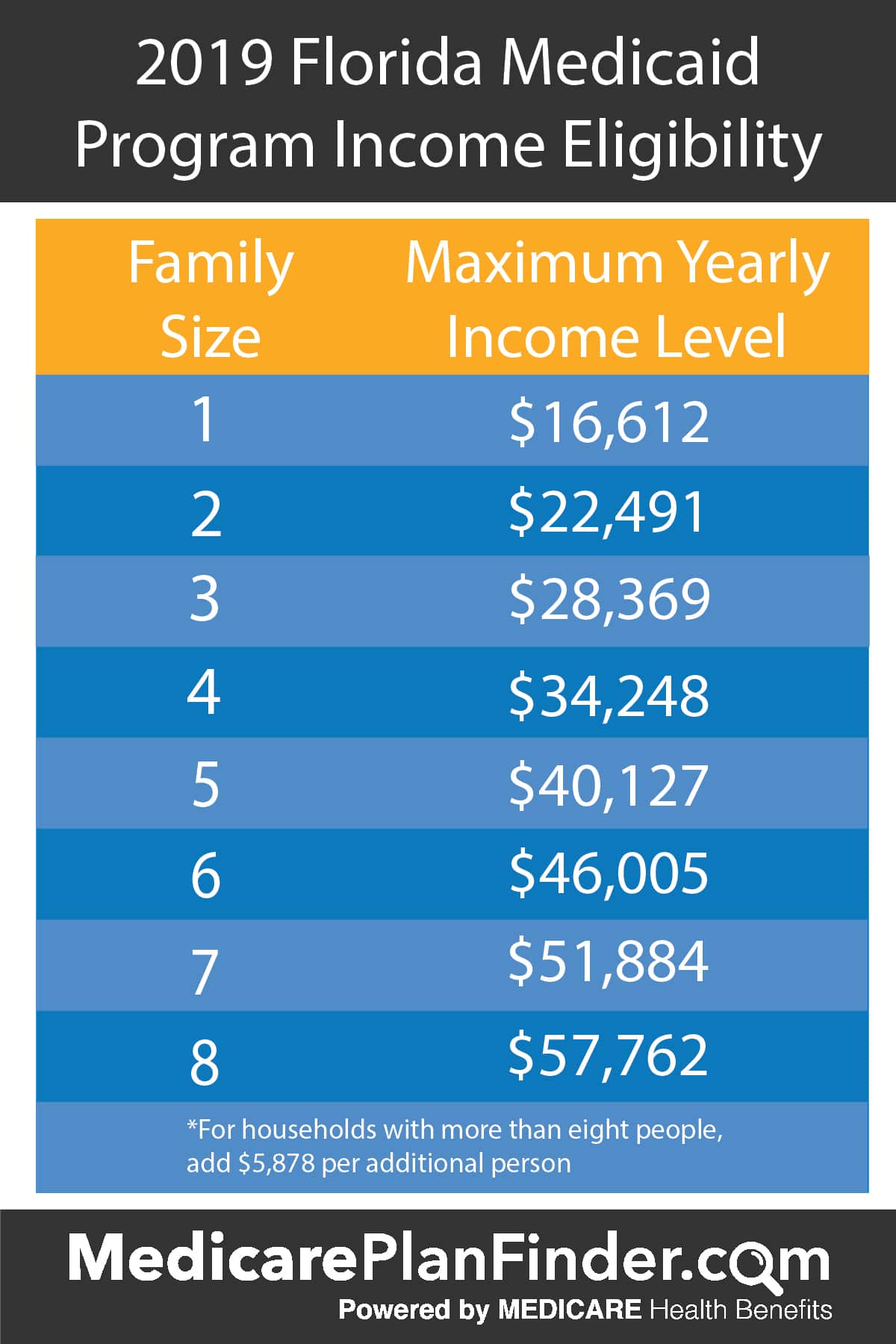
Income and Household Size
The primary factor for Medicaid eligibility is household income relative to the Federal Poverty Level (FPL). However, unlike states with expanded Medicaid, Florida does not offer coverage to all adults solely based on income below a certain FPL percentage. Instead, income limits vary significantly depending on the specific category an applicant falls into. For example, a pregnant woman or a child might qualify with a higher income than a non-disabled adult. These income thresholds are updated annually, so it’s essential to check the most current guidelines provided by the state.
When considering income, the state typically looks at your Modified Adjusted Gross Income (MAGI), which includes most taxable income and certain non-taxable income like Social Security benefits. It’s not just about your paycheck; it encompasses various sources of income for all members of your household. The household size also plays a critical role, as the income limits increase with more family members. For instance, a single parent with two children will have a different income threshold than a single adult without dependents. This detailed financial assessment ensures that the aid is directed to those who meet the strict criteria established by the program.

Specific Eligibility Groups
Beyond income, applicants must belong to one of the following specific eligibility groups to qualify for Florida Medicaid:
- Children: Children under the age of 19 are often eligible for Medicaid or the Children’s Health Insurance Program (CHIP), known as Florida KidCare. These programs have higher income thresholds, making coverage accessible to a broader range of families. Ensuring children have access to healthcare is a priority, especially for families planning a move or extended stay, providing peace of mind as they explore attractions like Universal Studios Florida or Busch Gardens Tampa Bay.
- Pregnant Women: Pregnant women can qualify for Medicaid coverage for services related to their pregnancy and for a period postpartum. This is a critical provision that supports maternal and infant health during a vulnerable time.
- Parents and Caretaker Relatives: In some cases, parents or caretaker relatives with dependent children may be eligible if their income is significantly low. This category often has very stringent income requirements due to Florida’s non-expansion status.
- Elderly (65 and Older): Seniors aged 65 and above may qualify for Medicaid, particularly if they have high medical expenses and limited income and resources. Medicaid can complement Medicare by covering costs not covered by Medicare, such as long-term care services.
- Individuals with Disabilities: People who meet the Social Security Administration’s definition of disability, regardless of age, can be eligible for Medicaid. This often requires a separate application process to determine disability status.
- Individuals Needing Long-Term Care: Medicaid is a primary payer for long-term care services, including nursing home care, home health services, and community-based care, for eligible individuals who meet medical and financial criteria. This is particularly relevant for retirees considering Florida as their permanent home.
- Medically Needy Program: Florida also offers a Medically Needy program, which allows individuals with significant medical bills to “spend down” their income to meet Medicaid eligibility thresholds. Once their medical expenses reduce their income to the Medically Needy income limit, they can qualify for coverage for the remainder of the month.
Residency and Citizenship Requirements
In addition to income and categorical requirements, applicants must meet certain residency and citizenship criteria. To qualify for Florida Medicaid, you must:
- Be a Florida Resident: You must intend to live in Florida and not just be visiting temporarily. This means establishing residency, which typically involves demonstrating an intent to remain in the state indefinitely.
- Be a U.S. Citizen, National, or Qualified Alien: Most applicants must be U.S. citizens or certain lawfully present immigrants. There are specific rules regarding immigrant eligibility, and certain immigrant groups may have waiting periods before they can qualify for full Medicaid benefits, although emergency Medicaid is often available regardless of immigration status.
It’s crucial to gather all necessary documentation to prove residency and citizenship during the application process. This might include utility bills, a Florida driver’s license, birth certificates, or immigration documents. For those moving from out of state, understanding these requirements upfront can streamline the application process and help them settle into their new Florida lifestyle more efficiently.
Navigating the Application Process
Applying for Medicaid in Florida involves several steps, but the process is designed to be accessible, offering multiple avenues for submission. Whether you prefer the convenience of online applications or the personal touch of in-person assistance, knowing your options and what to expect can significantly ease the journey. This section outlines the various methods available and the crucial documentation you’ll need to prepare.
Choosing Your Application Method
Florida offers flexibility in how you can apply for Medicaid, catering to different preferences and situations. For those who appreciate digital convenience, much like booking a stay at the Hyatt Regency Miami online, the primary method for applying is through the state’s online portal.
-
Online Application (Preferred Method): The most common and often quickest way to apply is through the Florida ACCESS website, managed by the Florida Department of Children and Families (DCF). This online portal allows you to create an account, complete your application, and upload required documents digitally. It’s available 24/7, making it convenient for applicants to submit their information from anywhere, whether they’re at home in Orlando or managing their affairs while considering a long-term stay in Jacksonville. The website provides step-by-step instructions and can guide you through the various sections, ensuring all necessary information is provided.
-
In-Person Application: If you prefer face-to-face assistance or have questions that are best answered in person, you can visit a local Florida Department of Children and Families (DCF) service center. These centers have staff available to help you complete the application, answer questions, and review your documents. This can be particularly helpful for individuals who may not be comfortable with technology or have complex situations requiring detailed explanations. You can find the nearest service center by searching the DCF website.
-
Mail Application: For those who prefer traditional methods, you can download a paper application from the Florida ACCESS website, fill it out, and mail it to the address provided on the form. While this method may take longer due to mailing times, it offers an alternative for individuals without internet access or those who prefer a physical record of their submission.
-
Phone Application: In some cases, you might be able to start an application over the phone, especially for simple renewals or to get initial guidance. However, a complete application typically requires submission through one of the other methods.
Gathering Essential Documentation
Regardless of how you choose to apply, having all your documentation prepared beforehand will significantly expedite the process. This is similar to preparing all your travel documents before an international trip or gathering booking confirmations for a stay at a luxury resort like The Ritz-Carlton, Amelia Island. Missing information is a common cause of delays. Here’s a list of typical documents you’ll need:
- Proof of Identity: A valid government-issued ID, such as a driver’s license, state ID card, or passport.
- Proof of U.S. Citizenship or Qualified Alien Status: Birth certificate, U.S. passport, naturalization certificate, or green card/immigration documents.
- Proof of Florida Residency: Utility bills, lease agreement, mortgage statement, or mail showing your Florida address.
- Social Security Numbers: For all household members applying for coverage.
- Proof of Income: Recent pay stubs (at least one month’s worth), tax returns, W-2s, Social Security benefit letters, unemployment benefit statements, or child support statements. This includes income for all household members.
- Proof of Assets/Resources (for certain categories): Bank statements, property deeds, or vehicle titles may be required, especially for elderly applicants or those seeking long-term care.
- Proof of Pregnancy (if applicable): A doctor’s note or medical record confirming pregnancy.
- Proof of Disability (if applicable): Documentation from a doctor or Social Security Administration (SSA) confirming disability status.
- Proof of Health Insurance (if any): Information about any existing health insurance coverage you or your family members may have.
- Child Care Expenses (if applicable): Receipts or statements for childcare costs.
It’s advisable to have copies of all these documents. If applying online, you’ll upload digital copies. If applying in person, bring the originals so staff can make copies. For mailed applications, send copies, not originals.
What Happens After You Apply?
Once your application is submitted, it will be reviewed by the Florida Department of Children and Families. This review process typically involves verifying the information you’ve provided, checking against state and federal databases, and possibly contacting you for additional details or clarification.
- Interview (if required): In some cases, you may be contacted for an interview, which can be conducted by phone or in person. This is an opportunity for the caseworker to ask questions and clarify any ambiguities in your application.
- Decision Notification: You will receive a written notification of the decision, informing you whether your application has been approved or denied. This letter will also explain the reason for the decision and provide information on how to appeal if you disagree with the outcome.
- Enrollment: If approved, you will typically receive information about how to enroll in a Medicaid managed care plan. Most Medicaid beneficiaries in Florida are required to enroll in one of these plans, which operate similarly to private health insurance, providing a network of doctors and hospitals. You’ll usually have a choice of plans, much like selecting preferred amenities at a resort like Four Seasons Resort Orlando at Walt Disney World Resort.
- Effective Date of Coverage: Coverage often begins retroactively to the date of your application or even up to three months prior if you had medical expenses during that period and were otherwise eligible.
The entire process can take several weeks, so it’s important to apply as soon as you anticipate needing coverage. Proactive planning ensures that you and your family can enjoy all aspects of Florida life, from the excitement of Kennedy Space Center Visitor Complex to the tranquility of its natural landscapes, with the assurance of accessible healthcare.
Benefits and Managing Your Coverage
Once you are approved for Medicaid in Florida, understanding the scope of your benefits and how to effectively manage your coverage is crucial for maximizing its utility. Medicaid is designed to be comprehensive, providing a wide array of medical services, but beneficiaries also have responsibilities to maintain their eligibility.
Comprehensive Healthcare Benefits
Florida Medicaid provides a robust package of healthcare services, ensuring that eligible individuals have access to the care they need. The specific services covered can vary slightly depending on the managed care plan you choose, but generally include:
- Doctor Visits: Coverage for primary care physicians, specialists, and preventative care.
- Hospital Stays: Inpatient and outpatient hospital services.
- Prescription Medications: A wide range of prescription drugs are covered, often with minimal or no co-payments.
- Emergency Services: Medically necessary emergency room visits.
- Mental Health Services: Counseling, therapy, and psychiatric care.
- Substance Abuse Treatment: Programs and services to address addiction.
- Dental Care: Typically covers routine check-ups, cleanings, fillings, and extractions for children, and limited emergency dental services for adults.
- Vision Care: Eye exams and, in some cases, eyeglasses for children; adult vision benefits may be limited.
- Laboratory and X-ray Services: Diagnostic tests and imaging.
- Home Health Services: Care provided in the home for eligible individuals.
- Transportation: Non-emergency medical transportation to and from appointments, if medically necessary.
- Medical Equipment: Durable medical equipment, such as wheelchairs or oxygen tanks, when prescribed.
These benefits offer a safety net, allowing individuals and families to focus on enjoying their life in Florida, rather than worrying about the cost of essential medical treatments. Whether you’re a new resident exploring local culture or a family enjoying the state’s countless attractions, knowing your healthcare is covered brings invaluable peace of mind.
Maintaining Your Medicaid Coverage
Being approved for Medicaid is the first step; maintaining your eligibility and coverage requires ongoing attention. Much like keeping track of your travel itineraries or accommodation bookings, staying organized with your Medicaid information is key.
- Annual Renewals: Medicaid eligibility is typically reviewed annually. You will receive a renewal notice in the mail or electronically, prompting you to re-verify your income, household size, and other eligibility factors. It is critical to complete and submit your renewal paperwork by the deadline to avoid a lapse in coverage.
- Reporting Changes: You are required to report any changes in your household circumstances to the Florida Department of Children and Families within a specified timeframe. This includes changes in income, employment, household size (e.g., birth of a child, someone moving out), residency, or other health insurance coverage. Failing to report changes could lead to an overpayment that you may have to repay or an incorrect termination of benefits. You can typically report these changes online through the Florida ACCESS website or by contacting your local DCF office.
- Choosing and Using Your Managed Care Plan: Most Florida Medicaid beneficiaries are enrolled in a managed care plan. It is important to understand your chosen plan’s network of providers, benefits, and procedures for referrals. You should contact your plan directly for any questions regarding your specific coverage or to find in-network doctors and facilities.
- Keeping Contact Information Updated: Ensure that the Florida Department of Children and Families has your current mailing address and phone number so you don’t miss important notices regarding your coverage.
By staying proactive and informed, you can ensure your Medicaid benefits remain active, providing continuous access to the healthcare services you need while enjoying all that Florida has to offer. This diligence allows for a truly relaxed and secure lifestyle, whether you’re exploring the bustling avenues of Miami or the serene landscapes of the panhandle.
Accessing healthcare should not be an insurmountable barrier, especially for those who call Florida home or plan to do so for an extended period. While the eligibility requirements for Medicaid in the Sunshine State can be specific, they are designed to provide a vital safety net for its most vulnerable residents. By understanding the criteria, diligently preparing your application, and proactively managing your coverage, you can secure essential medical care for yourself and your family. This foundational step ensures that as you settle into the vibrant Florida lifestyle, whether it’s for a long-term stay, a new career, or enjoying retirement, your health needs are met, allowing you to fully embrace the opportunities and experiences this incredible destination has to offer. Remember, help is available through the Florida Department of Children and Families and various community organizations should you need assistance with your application.
LifeOutOfTheBox is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. Amazon, the Amazon logo, AmazonSupply, and the AmazonSupply logo are trademarks of Amazon.com, Inc. or its affiliates. As an Amazon Associate we earn affiliate commissions from qualifying purchases.